You’ve been told that your tooth cannot be saved and now needs to be removed. Next, you have to make a decision regarding what the best course of treatment is for you. With all of the advancements in modern dentistry, the options for replacing teeth can seem endless. Well, before you decide, let’s talk about what happens to the bone at the extraction site.
When a tooth is removed, it triggers an immune response of alveolar jaw bone resorption, or “melting away” of the jaw. Basically, the function of bone in the jaw is to provide facial structure and support for your teeth. After the loss of a tooth, there is no more bone stimulation by the tooth roots, so the body’s response is to dissolve or melt away the bone and its blood supply. The loss of this bone mass can change the shape of your face and fullness of your smile, giving a prematurely aged look (See Figure 1).
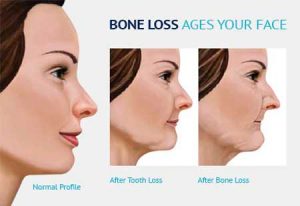
The key to preventing this bone loss and subsequent aged look is to replace the tooth root that was stimulating the jaw bone. There is only one option for replacing the tooth root, and that is placing a dental implant at the extraction site.
Dental implants can change your life. They not only replace missing teeth, but more importantly, they preserve facial bone structure. Like teeth, dental implants provide stimulation to the bone, maintaining bone and blood supply in the area. While dental implants can maintain bone, sufficient bone is needed to begin with for placement of a dental implant.
To provide sufficient jaw bone density, it is recommended that an alveolar ridge augmentation or socket preservation (bone graft) be performed during the tooth extraction procedure. This allows the transplanted bone to use the body’s blood supply and the immune response to transform this bone into the patient’s own healthy bone (See Figure 2). This preliminary bone graft is important because it prepares the extraction site for dental implant placement by regenerating and maintaining healthy and strong bone structure. The timing of the bone graft and dental implant placement is important as the majority of bone resorption occurs between 12 and 18 months after tooth removal. After this time span, a secondary bone graft may be necessary.
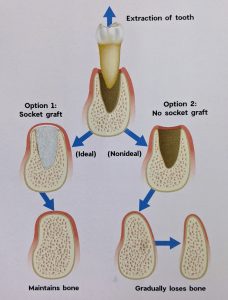
There are several types of bone to regenerate this healthy new bone. An autograft is bone from the patient’s jaw transplanted from any area of excess bone to the area lacking bone. Since the bone is taken from the site of excess bone, this type of bone graft usually requires a second surgical site. A more common type of graft material is an allograft, which is cortical and cancellous bone from a tissue donor. The safety testing on this donor bone is unparallelled in medicine.
Approximately 6 weeks after the bone regeneration procedure is performed, the transplanted bone is completely remodeled into the patient’s own new healthy bone. Typically, a cone beam CT scan may be needed to confirm that there is sufficient bone, and if sufficient bone density is confirmed, the jaw can now function to support a dental implant, which in turn will function to replace the missing tooth and maintain jaw bone structure.
The number of bone graft procedures performed at the time of tooth extraction is over 2.2 million per year worldwide. This additional bone has enabled implant placement procedures worldwide to have a greater than 96% success rate. This is the most successful medical implant procedure performed globally. Discussing this option with your dentist prior to tooth removal is paramount to making an informed decision about your oral health.


